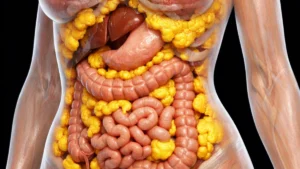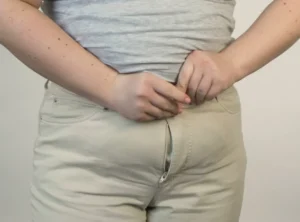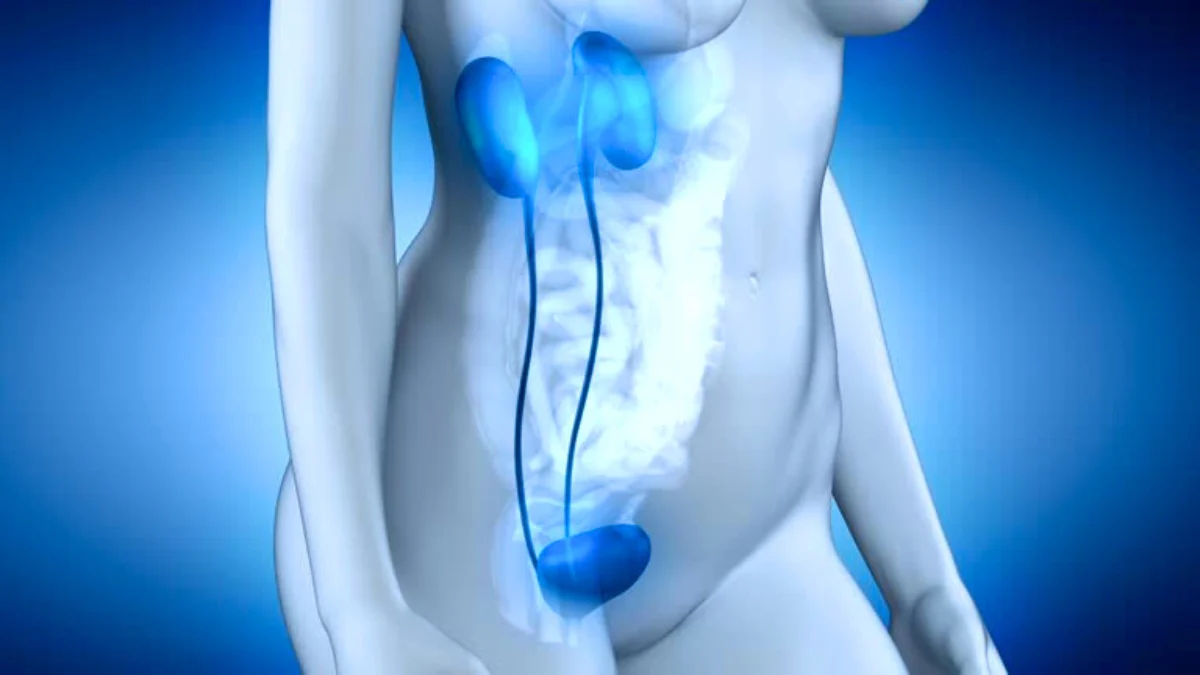
Why Does Urinary Incontinence Occur During Menopause?
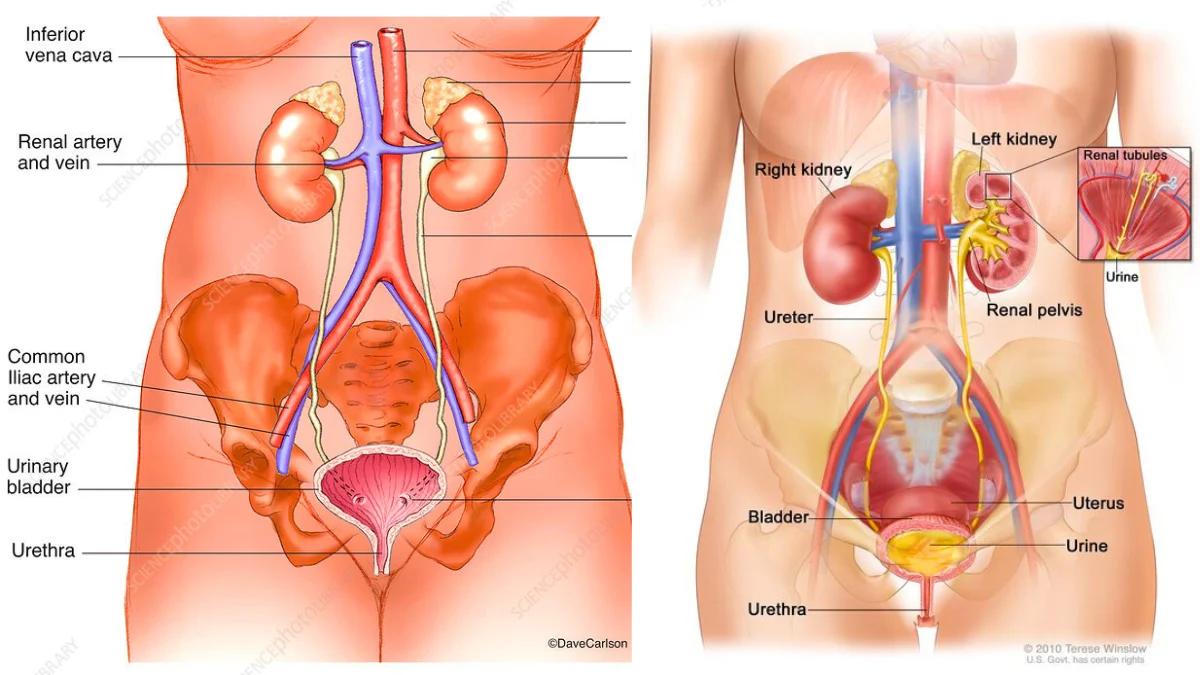
The Role of Estrogen
According to the website “Disrupt Hormones,” during menopause, estrogen levels drop drastically. This hormone is essential for maintaining the health of the tissues in the urinary tract. Estrogen keeps the urethra and bladder hydrated, elastic, and strong.
When estrogen decreases, the tissues of the urethra and the base of the bladder become thinner, drier, and less elastic. This weakens the urethral closure mechanism, allowing urine to leak involuntarily.
Weakening of Pelvic Floor Muscles
Inflammation of the Urinary Tract
Types of Incontinence During Menopause
Adequate Hydration - The Foundation of Everything

Why Is Drinking Water Essential?
The Hydrating Action of Water
How Much to Drink?
When to Drink
Practical Tips
Signs of Good Hydration
Uva Ursi - The Ancient Natural Remedy

What Is Uva Ursi?
Anti-inflammatory Properties
Antiseptic Properties
How to Use Uva Ursi
Duration of Treatment
Safety and Contraindications
Pelvic Floor Exercises - Muscle Strengthening
Why Are Pelvic Floor Muscles Important?
How Pelvic Floor Exercises Work
How to Find the Correct Pelvic Floor Muscles
Basic Kegel Exercise
Exercise Progression
Advanced Exercise – Quick Contractions
When to Expect Results
Tips for Success
Signs You’re Doing It Right
Signs You Might Be Doing It Wrong
Combining All Three Solutions

Complete Protocol
Expected Results
Other Important Tips
Lifestyle
Safety and Precautions
When to Consult a Doctor
Hydration
Uva Ursi
Pelvic Floor Exercises
Conclusion
Urinary incontinence during menopause is a common but treatable problem. You don’t have to suffer in silence or accept it as an inevitable part of menopause.
But this article is for informational purposes only.
It does not eliminate the need to consult a doctor, pharmacist, and physiotherapist.
The three natural solutions I shared adequate hydration, uva ursi, and pelvic floor exercises are proven by scientific research and have been used for centuries.
Many women have regained full bladder control using these natural strategies. You can too.
Remember: you are not alone. More than 50% of postmenopausal women face this problem. It’s time to talk openly about it and seek solutions.
Your quality of life deserves to be restored. Start today.
Scientific References
Written and reviewed by: Dr. Vilma Mendonça – Pharmacist
Image bank – Pexels, Yandex, IA