
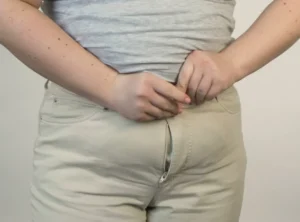
What Is Menopause Belly?
Menopause belly is one of the most frustrating changes many women experience often without warning and without any clear reason.
If your belly has grown during menopause, even though your habits haven’t changed, you are not imagining it.
And more importantly: it’s not your fault.
This is a real biological process driven by hormonal changes, especially the drop in estrogen and the rise of cortisol. Understanding menopause belly is the first step to managing it effectively without extreme diets or unrealistic expectations.
The Science Behind Menopause Belly
Why Does Fat Move to the Belly During Menopause?
For most of your life, your body followed a hormonal “map” and estrogen was the one drawing it.
One of estrogen’s lesser-known roles is deciding where fat is stored. Under its influence, fat is usually stored in the hips, thighs, and buttocks. This type of fat is called subcutaneous fat, and it’s actually less harmful to your health.
But during menopause, estrogen levels drop.
And when that happens, your body changes strategy.
Instead of storing fat in those “safer” areas, it begins to store fat around the abdomen especially visceral fat, which surrounds your internal organs.
👉 That’s why your belly may grow even if nothing else changes.
And no you’re not imagining it.
Visceral Fat vs Subcutaneous Fat: Why It Matters
This is not just about appearance.
Visceral fat behaves very differently from subcutaneous fat.
While subcutaneous fat sits under the skin, visceral fat is metabolically active, meaning it constantly releases substances into your bloodstream.
This leads to:
- Increased inflammation
- Higher risk of insulin resistance
- Greater difficulty losing weight
And here’s where the cycle begins…
Insulin Resistance: The Silent Driver
As visceral fat increases, your body becomes less sensitive to insulin — the hormone that helps move sugar from your blood into your cells.
To compensate, your body produces more insulin.
And here’s the problem:
👉 High insulin levels promote fat storage especially in the belly.
So now you have a loop:
- More belly fat → more insulin resistance
- More insulin → more belly fat
And the cycle continues.
The Cortisol Connection: Why Stress Targets Your Belly

If estrogen starts the problem, cortisol makes it worse.
Cortisol is your body’s stress hormone. It’s useful in short bursts — but when it stays elevated for too long, it becomes a major driver of belly fat.
And menopause creates the perfect storm for that.
You may be dealing with:
- Poor sleep due to night sweats
- Mood swings and anxiety
- Daily stress from work and family
- Internal inflammation
All of this keeps cortisol levels high.
How Cortisol Increases Belly Fat
Cortisol affects your body in several ways:
- Increases cravings (especially sugar and carbs)
- Promotes fat storage in the abdominal area
- Worsens insulin resistance
- Disrupts deep sleep
And poor sleep creates another problem:
👉 Your body produces less growth hormone which is essential for fat burning and muscle maintenance.
The result?
A slower metabolism… and more fat stored around the belly.
Natural Pharmacy Solutions: Evidence-Based Supplements

Science-Based Support: Natural Compounds That Can Help
Before we talk about solutions, it’s important to be clear:
👉 There is no magic pill.
But there are evidence-based tools that can support your metabolism especially when combined with lifestyle changes.
Three stand out in research:
- Berberine
- Inositol
- Magnesium
Within the vast universe of natural supplements, three compounds have accumulated a growing body of scientific evidence with direct relevance to the mechanisms described above: berberine, inositol and magnesium. For a broader view of how natural compounds can support this transition, it’s worth reading our guide on natural remedies and menopause symptoms.
Berberine — The “Natural Ozempic”?
Berberine is a plant alkaloid present in plants such as Berberis vulgaris, used for centuries in traditional Chinese medicine. Its main mechanism of action involves AMPK activation (AMP-activated protein kinase), an enzyme often described as the “master metabolic switch” of the cell. AMPK activation improves insulin sensitivity, stimulates glucose uptake by muscles, reduces hepatic glucose production and promotes fatty acid oxidation.
Clinical studies published in peer-reviewed journals have demonstrated significant reductions in fasting blood glucose, glycated haemoglobin (HbA1c) and triglycerides in participants with insulin resistance. In some direct comparisons with metformin the reference drug for insulin resistance berberine showed comparable efficacy in glycaemic control, which is remarkable for a natural compound. It does not replace prescribed medication, but may constitute relevant metabolic support under medical supervision.
Inositol — The Silent Regulator of Insulin
Inositol, particularly myo-inositol, functions as an intracellular second messenger in insulin signalling. When this compound is deficient a situation observed in menopausal women the insulin signalling cascade becomes impaired, contributing to hormonal resistance.
Available scientific evidence demonstrates that myo-inositol supplementation (typically at doses of 2 to 4 grams daily) improves insulin sensitivity, reduces fasting insulin levels and may have a favourable effect on lipid profile. For menopausal women with documented insulin resistance, inositol represents a natural option with a favourable safety profile and few known side effects.
Magnesium — The Mineral of Sleep, Cortisol and Metabolism
If there were a single supplement to recommend at this stage of life, magnesium would be one of the strongest candidates. This essential mineral participates in more than 300 enzymatic reactions in the human body, and its deficiency surprisingly common, estimated to affect 50 to 60% of the Western population has direct consequences in three critical areas for combating menopause belly.
First, cortisol control: magnesium regulates the hypothalamic-pituitary-adrenal (HPA) axis, which governs the stress response. Adequate magnesium levels act as a natural “buffer” for the cortisol response. Second, sleep quality: magnesium activates the parasympathetic nervous system and increases GABA levels, promoting deeper, more restorative sleep. Third, insulin sensitivity: magnesium is a cofactor of enzymes involved in glucose metabolism and insulin signalling its deficiency directly worsens insulin resistance.
The most bioavailable and studied forms are magnesium glycinate (particularly effective for sleep and stress), magnesium malate and magnesium taurate.
Quick Checklist: Do You Have Menopause Belly?
- Increased belly fat without lifestyle changes
- Difficulty losing weight
- Frequent bloating
- Poor sleep
- Increased cravings
There are several ways to manage symptoms including natural approaches, which you can explore in our guide on menopause natural remedies.
Lifestyle Over Dieting: Movement That Actually Works

Why Restrictive Diets Are Counterproductive in Menopause
Simple 5-Step Strategy to Reduce Menopause Belly
- Prioritize protein in every meal
- Walk daily (20–30 minutes)
- Improve sleep quality
- Manage stress (breathing, yoga)
- Support metabolism with key nutrients
Severe low-calorie diets, especially those that drastically cut carbohydrates or total calories, have a particularly destructive effect on the metabolism of menopausal women. The reason is straightforward: aggressive caloric restriction promotes muscle mass loss. And in menopause a phase where the decline in oestrogen already naturally reduces muscle protein synthesis losing muscle means directly slowing basal metabolism. The classic result is the yo-yo effect: weight is lost short-term (mostly muscle and water), and regained with interest (predominantly abdominal fat).
It is also worth noting that visceral fat triggers a persistent low-grade inflammatory response in the body. Understanding how to reduce that internal inflammation through nutrition and lifestyle is a topic we explore in depth in our article on natural anti-inflammatories in menopause.
Gentle, Joint-Friendly Movement: What Science Recommends
Many menopausal women experience joint pain, bone sensitivity and general body discomfort making high-impact exercise not only unappealing but often genuinely inadvisable. The good news is that the most effective movement for this phase of life is also among the gentlest. Three modalities stand out both in scientific literature and in clinical practice:
Yoga
Yoga addresses menopause belly from multiple angles simultaneously. Beyond the physical benefits of improved flexibility and gentle muscle toning, yoga has clinically documented effects on cortisol reduction and sleep quality two of the central mechanisms driving abdominal fat accumulation in menopause.
Scientific evidence: A study published in Menopause: The Journal of the Menopause Society (Afonso et al., 2012) demonstrated that a 4-month yoga programme significantly reduced menopausal symptoms, including sleep disturbances and anxiety, in postmenopausal women directly targeting the cortisol-belly fat connection. A randomised controlled trial published in the Journal of Mid-Life Health (Shantakumari et al., 2020) found significant improvements in body composition, fasting glucose and perceived stress in menopausal women following a structured yoga protocol.
Walking
Brisk walking is one of the most underrated yet scientifically validated interventions for visceral fat reduction. It is accessible, low-impact, requires no equipment and can be adapted to any fitness level. Crucially, regular walking improves insulin sensitivity, helps regulate blood sugar levels and reduces systemic inflammation directly addressing the core metabolic disruption of menopause belly.
Scientific evidence: A study published in the International Journal of Obesity (Asikainen et al., 2004) found that brisk walking 4 to 5 times per week for 24 weeks produced significant reductions in visceral fat and improvements in cardiovascular risk markers in postmenopausal women, independently of dietary changes.
Pilates
Pilates offers a uniquely appropriate combination of core strengthening, postural correction and controlled breathing without the joint stress associated with more intense forms of exercise. The deep abdominal and pelvic floor engagement characteristic of Pilates has been shown to improve body composition, reduce waist circumference and enhance quality of life in menopausal women, while also addressing the postural changes that frequently accompany this phase.
Scientific evidence: A randomised controlled trial published in the Journal of Bodywork and Movement Therapies (Rodrigues et al., 2011) demonstrated that a 16-week Pilates programme significantly reduced waist circumference and improved functional capacity in postmenopausal women, with no adverse joint effects reported.
Pharmacist's Warning: The Most Important Section of This Article

All information shared in this article has a scientific basis and has been prepared with rigour but there is a step that cannot be skipped before starting any supplement: consulting your doctor or pharmacist.
Berberine, in particular, presents clinically relevant drug interactions that must not be underestimated. It can potentiate the effect of oral antidiabetics (such as metformin) and insulin, with risk of hypoglycaemia; it interferes with the hepatic metabolism of several drugs through cytochrome P450 enzymes (CYP3A4 and CYP2D6); it may interact with anticoagulants such as warfarin, increasing haemorrhagic risk; and it should not be used simultaneously with cyclosporine or other immunosuppressants without rigorous medical monitoring.
Inositol is generally well tolerated, but at high doses may cause gastrointestinal effects; women with hypothyroidism should inform their doctor before starting supplementation. Magnesium, despite its excellent safety profile, may interact with fluoroquinolone and tetracycline antibiotics (reducing their absorption), with bisphosphonates used in osteoporosis, and may have a laxative effect at high doses.
Beyond drug interactions, it is essential to emphasise that symptoms such as rapid abdominal fat accumulation, persistent fatigue, significant mood changes and sleep disturbances deserve medical evaluation not only to confirm that this is “normal” menopause, but to rule out conditions such as hypothyroidism, Cushing’s syndrome or severe insulin resistance that require specific therapeutic management.
Self-medication is never harmless. “Natural” does not automatically mean “safe for everyone”. What this article offers is scientific literacy the ability to arrive at your appointment with the right questions and have a more informed conversation with your doctor. The therapeutic decision always belongs to the clinical team that accompanies you.
Conclusion
Menopausal belly is not inevitable, nor is it a permanent sentence. It is the visible expression of a set of hormonal and metabolic changes that have identifiable causes and, therefore, have solutions. Not quick fixes, nor miracle pills, but science-based interventions: understanding the role of estrogen and cortisol, considering scientifically proven supplements under medical supervision, abandoning the mindset of restrictive diets once and for all, and adopting gentle and consistent exercise and a protein-rich diet as the pillars of a healthy metabolism at this stage .
Your body has changed. The strategy also needs to change. And that change begins with information. Always consult your doctor for the best assessments. https://mariahchic.com/menopause/abdominal-fat
FAQs
Can menopause belly go away?
Yes, with the right approach focused on hormones, lifestyle, and metabolism.
Why do I gain belly fat during menopause?
Due to hormonal changes, especially lower estrogen and higher cortisol levels.
What is the best exercise for menopause belly?
Walking, yoga, and strength training are highly effective.
How long does it take to lose menopause belly?
It depends on consistency, but changes can begin within weeks.
Are supplements necessary?
Not always, but some can support metabolism when used correctly.
Is menopause belly permanent?
No it can be managed and reduced with the right strategy.
More information: https://www.ncbi.nlm.nih.gov/
Scientific Studies:
Asikainen, T.M., Kukkonen-Harjula, K., & Miilunpalo, S. International Journal of Obesity — 2004
Afonso, R.F., Hachul, H., Kozasa, E.H., et al. Menopause: The Journal of the Menopause Society — 2012
Written and reviewed by: Dr. Vilma Mendonça – Pharmacist
AI Images





1 Comment
[…] If you want to understand the full hormonal and metabolic mechanisms behind this process, you can read our complete guide on menopause belly here:👉 https://mariahchic.com/menopause/menopause-belly/ […]