Reviewed by Pharmacist Vilma Mendonça, CRF 9930RJ — Specialist in Phytotherapy and Homeopathy
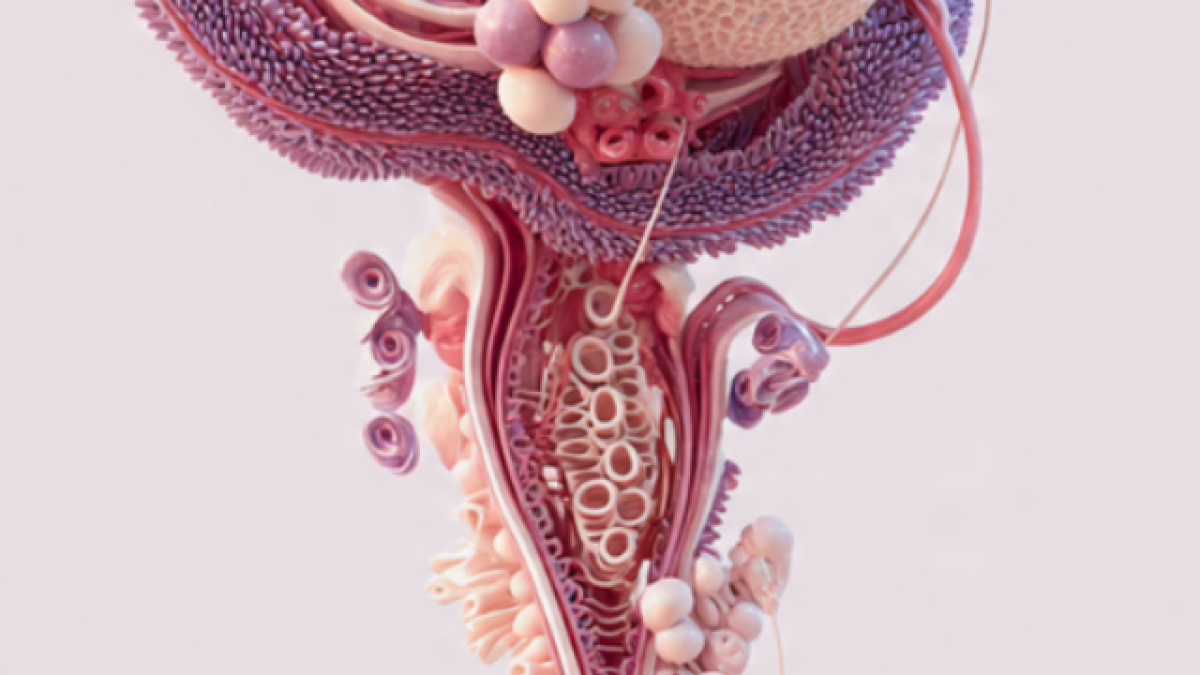
There is a symptom that affects more than half of all women. After menopause and most of them suffer in silence for years before ever mentioning it to a doctor.
Vaginal dryness. Not just dryness during sex. Daily dryness. The kind that makes wearing certain clothes uncomfortable. The kind that causes burning when you sit for too long. The kind that wakes you up at night with itching. The kind that quietly erodes your confidence. Your relationship, and your quality of life while you tell yourself it is just part of getting older and you should learn to live with it.
You should not have to live with it. And you do not have to.
This article goes beyond the basics. See your doctor whenever you feel it’s necessary for any necessary tests and medication. If you already know that a drop in estrogen causes vaginal dryness. This article doesn’t end there. We’ll talk about what really happens inside your tissue. Why the problem worsens if left untreated. What the latest research says about natural approaches, and why the connection between the gut and hormones. Might be the missing piece that most women have never heard of.
What Is Actually Happening to Your Tissue
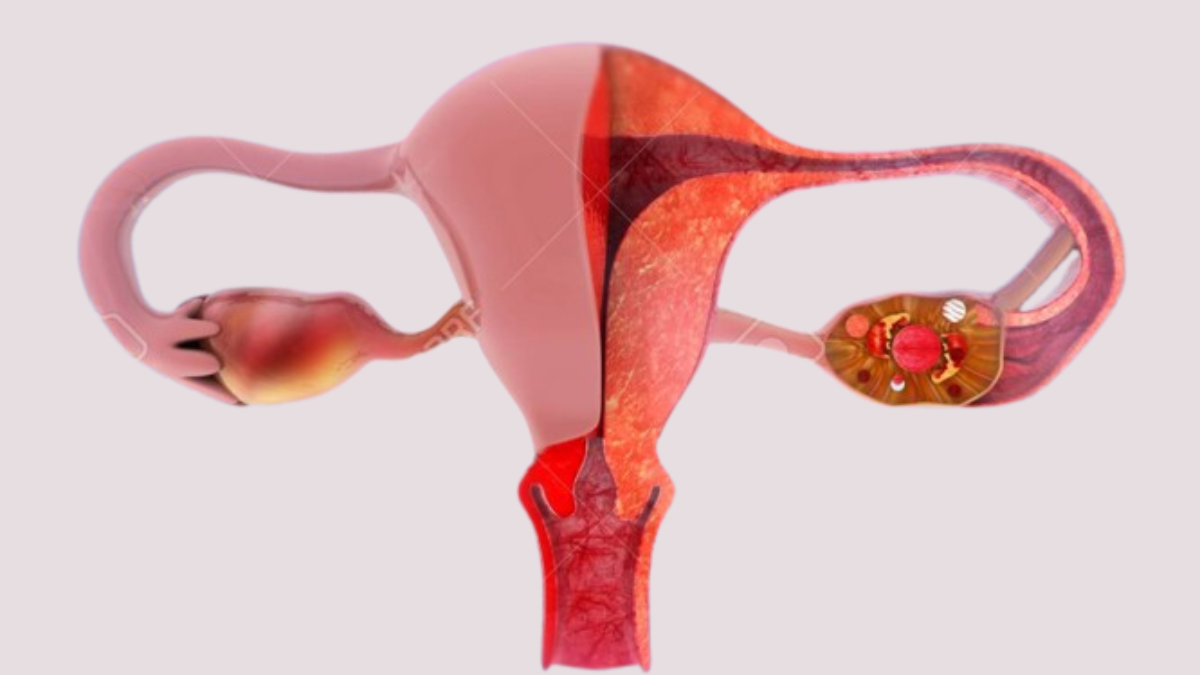
The medical term is Genitourinary Syndrome of Menopause or GSM. The name changed from the older “vaginal atrophy” because researchers realized the condition affects far more than just the vagina. It affects the vulva, the bladder, and the urethra as well.
Here is what happens at the tissue level when estrogen declines:
The vaginal wall has three layers. Estrogen keeps all three healthy, thick, and well-supplied with blood. When estrogen drops, the innermost layer the epithelium begins to thin. The cells that used to regenerate every few weeks now regenerate more slowly. The tissue loses collagen (yes, the same collagen that affects your skin and joints). It loses elasticity. The small blood vessels that used to keep tissue moist and resilient become less active.
In a Healthy Premenopausal Vagina pH
At the same time, the vaginal pH rises. In a healthy premenopausal vagina, pH is acidic around 3.5 to 4.5. That acidity protects against harmful bacteria. When estrogen drops and pH rises toward 5, 6, or higher, the protective environment breaks down. Harmful bacteria and yeast thrive. This is why many women experience recurring infections alongside vaginal dryness it is not coincidence. It is the same root cause.
The critical insight: GSM is progressive. Unlike hot flashes, which often reduce in intensity over time. Vaginal dryness tends to worsen as the years pass after menopause unless actively addressed. The women who wait often find that symptoms that were manageable at 52 become significantly more disruptive at 58.
The Symptoms Beyond Dryness That Most Women Don't Recognize
Vaginal dryness rarely presents as just one symptom. Most women experience a cluster but because they do not know. The symptoms are connected, they treat each one separately without addressing the root cause.
Vaginal and vulvar symptoms include dryness, itching, burning, a feeling of pressure or tightness, and increased sensitivity to clothing, underwear elastic, or exercise. The tissue can feel fragile small amounts of friction that were previously unnoticed now cause irritation.
Sexual symptoms include pain during intercourse (dyspareunia), reduced arousal, and decreased ability to reach orgasm. Many women quietly withdraw from intimacy without explaining. Why which creates distance in relationships that both partners struggle to understand.
Urinary symptoms are the ones most women never connect to vaginal dryness. Because the same estrogen decline that affects vaginal. Tissue also thins the lining of the bladder and urethra, many women develop increased urinary urgency. The frequency, and a higher rate of urinary tract infections. If you have had more UTIs in the past two or three years than in the previous decade, GSM may be a significant factor.
The Gut-Hormone Connection: The Missing Piece
This is the part most articles skip and it may be the most important for women who prefer natural approaches.
Inside your gut lives a specific collection of bacteria called the estrobolome. These bacteria produce an enzyme called beta-glucuronidase, which plays a direct role in how your body. Processes and recirculates estrogen. When your estrobolome is healthy and diverse, it helps maintain estrogen metabolism efficiently. When it is imbalanced due to poor diet, antibiotics, stress, or low fiber intake estrogen metabolism becomes disrupted.
For women in perimenopause and menopause, this matters enormously. A disrupted estrobolome means that whatever estrogen. Your body is still producing is not being metabolized and recirculated effectively. The result is lower circulating estrogen levels which means dryer, thinner vaginal tissue.
What supports the estrobolome:
- Fiber from vegetables, legumes, and whole grains feeds beneficial bacteria
- Fermented foods (yogurt with live cultures, kefir, sauerkraut) introduce diverse bacteria
- Prebiotic foods (garlic, onion, asparagus, green banana) feed the bacteria already there
- Reducing ultra-processed foods and excess sugar which feed harmful bacteria
This is not a quick fix. But women who improve gut health as part of a broader approach to menopause. Symptoms consistently report better hormonal balance across multiple symptoms not just vaginal dryness.
Phytoestrogens and vaginal tissue: what recent research shows
Phytoestrogens have been discussed in menopause circles for years. But the research has become considerably more specific in recent years. Particularly around their direct effect on vaginal tissue.
Soy isoflavones (genistein and daidzein) have been the most studied. A 2025 systematic review confirmed that consistent. Supplementation with 40–80mg of soy isoflavones daily over 12 weeks. Produces measurable improvements in vaginal tissue hydration and reduced dyspareunia (pain during sex) in postmenopausal women. The key word is consistent these are not immediate-relief compounds. They work by gradually supporting the tissue over time.
Pueraria mirifica, a plant native to Thailand and Myanmar with unusually high phytoestrogenic activity. Has shown particularly strong results in several recent trials for vaginal tissue specifically. Unlike soy isoflavones, it appears to act more directly on vaginal epithelium. However, because of its potency. It requires caution and professional guidance especially for women with a history of hormone-sensitive conditions.
Topical vitamin E applied directly to vaginal tissue has solid evidence behind it. A 2024 randomized controlled trial found that vitamin E vaginal suppositories used three times weekly for 8 weeks. Significantly reduced dryness, itching, and pain compared to placebo with no systemic hormonal effects. This is a practical, accessible option for many women.
Pharmacist’s Note — Vilma Mendonça, CRF 9930RJ: For a comprehensive overview of the main phytohormones used for vaginal dryness. Use including soy isoflavones, red clover, black cohosh, and flaxseed lignans with their mechanisms, benefits, and safety. Warnings, read our detailed guide: Why Vaginal Dryness Happens in Menopause. The information in this article is designed to complement, not replace, that foundational resource.
Nutrition Specifically for Vaginal Tissue Health

Beyond phytoestrogens, specific nutritional strategies support vaginal tissue integrity from the inside.
Omega-3 fatty acids (from fatty fish, flaxseed, and fish oil supplements) reduce the inflammatory environment that worsens GSM symptoms. Chronic low-grade inflammation which accelerates during menopause directly compromises tissue integrity and moisture.
Vitamin D has estrogen receptor-modulating effects throughout the body, including in vaginal tissue. Many women with severe GSM symptoms are found to be significantly vitamin D deficient. Optimizing vitamin D levels (target: 40–60 ng/mL) is a foundational step that is frequently overlooked.
Collagen-supporting foods vitamin C-rich vegetables, bone broth, and adequate dietary protein support the connective tissue of vaginal. Walls just as they support skin and joint cartilage. The vaginal wall contains collagen. When the body lacks the raw materials to produce it, tissue thins faster.
Hydration is simple but underestimated. Vaginal tissue moisture is directly influenced by systemic hydration. Women who are chronically mildly dehydrated a common state. Particularly in women over 45 experience more severe dryness symptoms. Aim for at least 1.5 to 2 liters of water daily.
What to Avoid: Factors That Accelerate GSM
As important as what you add is what you remove:
Fragranced products soaps, washes, wipes, and sprays used in the vaginal area disrupt pH and damage already fragile tissue. The vagina is self-cleaning. It requires water only nothing else.
Smoking significantly reduces blood flow to pelvic tissue, accelerating the very tissue thinning that causes dryness and pain. Women who smoke reach more severe GSM symptoms earlier than non-smokers.
Alcohol has a drying effect systemically and disrupts sleep, which affects the hormonal recovery that happens during deep sleep phases.
High sugar intake feeds harmful bacteria in both the gut and the vaginal microbiome, increasing infection risk and worsening the pH imbalance already caused by estrogen decline.
When Natural Approaches Are Not Enough
Natural approaches work well for mild to moderate symptoms, and for women who want to prevent progression before symptoms become severe. But they have limits.
When vaginal dryness is causing significant pain during intercourse, daily discomfort. That affects movement and activity, or recurring urinary tract infections, it is time to discuss medical options with a healthcare professional.
Low-dose vaginal estrogen available as creams, tablets, rings, or suppositories delivers estrogen directly to the tissue with minimal systemic absorption. It is considered the most effective treatment for moderate to severe GSM, and current guidelines confirm it can be used safely long-term.
There is no virtue in suffering through severe symptoms when effective treatment exists. Managing menopause well naturally where possible, medically where necessary is not a compromise. It is wisdom.
A Practical Daily Protocol for Vaginal Tissue Health

Daily HabitWhat It Does1.5–2L waterSystemic hydration reaches vaginal tissue. Omega-3 supplement or fatty fishReduces tissue inflammation. Fermented food (yogurt/kefir)Supports estrobolome and estrogen metabolism25–30g fiber from foodFeeds beneficial gut bacteria. Vitamin D (check levels first) Supports estrogen receptor activity in tissue.
Remove fragranced intimate productsProtects fragile tissue and pH balance. Topical vitamin E (3x/week if needed)Direct tissue hydration without hormonal effect
Conclusion
Vaginal dryness in menopause is not a minor inconvenience. It is a progressive, treatable condition that affects more than half of postmenopausal.
Women most of whom never seek help because they believe. There is nothing to be done, or because the topic feels too private to raise.
The most powerful thing you can do is understand what is happening in your body and act before the symptoms become severe. The gut-hormone connection, phytoestrogens, targeted nutrition, and the elimination of irritants form a comprehensive natural. Strategy that can meaningfully reduce symptoms and slow progression.
You deserve to be comfortable in your body. At every age.
Related article:
Scientific References
- Cyriac J, Sood R. Case-Based Perspectives on the Management of Genitourinary Syndrome of Menopause. Gynecology. 2026;16(3):60. doi:10.3390/gynecology16030060 — PMC
- Portman DJ, Gass ML; Vulvovaginal Atrophy Terminology Consensus Conference Panel. Genitourinary syndrome of menopause: new terminology for vulvovaginal atrophy from the International Society for the Study of Women’s Sexual Health and The Menopause Society. Menopause. 2014;21(10):1063–1068. doi:10.1097/GME.0000000000000329 — PubMed
© Mariah Chic — Menopause Health & Natural Solutions for Women Over 45 Reviewed by Pharmacist Vilma Mendonça, CRF 9930RJ — Specialist in Phytotherapy, Homeopathy and Cosmetology
IA Image